EPIDURAL ABSCESS
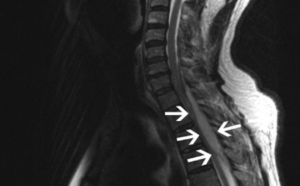
What’s an Epidural Abscess?
An epidural abscess refers to a collection of pus and infectious material located in the epidural space superficial to the dura mater which surrounds the central nervous system. Due to its location adjacent to the brain or spinal cord, epidural abscesses have the potential to cause weakness, pain and paralysis.
In other words, an epidural abscess refers to an infection within the epidural space anywhere in the brain or spinal cord. Dura mater makes up the internal lining of the bony skull, and under normal conditions, no space occurs between the skull and the dura mater. Increased intracranial pressure (ICP) related to infections, inflammation or tumors opens up the epidural space and separates the bone from the tissue.
This newly formed, pathological epidural space may contain blood, pus, or an abscess. Below the foramen magnum, the epidural space extends the length of the vertebral column. It has 2 compartments:
- A true space posterior and lateral to the spinal cord containing a cushioning layer of fat embedded with perforating arteries and an extensive venous plexus.
- A potential anterior space where the dura mater attaches to the posterior surface of the vertebral body.
Epidural abscesses occur as a result of infections involving the cranial or spinal epidural space. Intracranial epidural abscesses (IEA) refer to complications of cranial surgery or trauma; these may also complicate otorhinolaryngological (ear, nose and throat) infections or other neck and thoracic procedures. Spinal epidural abscess (SEA) can have an acute and chronic presentation. This simple categorization correlates with certain clinical and laboratory manifestations, bacteriological and cerebrospinal fluid (CSF) formulae, anatomic details and pathology.
Acute spinal epidural abscess occurs usually less than 2 weeks in duration with fever and signs of systemic inflammation from a hematogenous source. This contrasts with subtle, afebrile, and long-standing chronic spinal epidural abscess that results from a direct extension of vertebral osteomyelitis. Both forms present with radicular pain, but leukocytosis (in serum and CSF) occurs more likely in the acute form and not so much in the chronic form. Acute forms usually occur posterior to the spinal cord, unlike chronic forms, which commonly occur anterior to the spinal cord.
What causes an Epidural Abscess?
Typically, a Staphylococcus aureus bacterial infection presents as the cause of an epidural abscess. It could also result from a fungal infection or another germ circulating in the body.
IEA usually starts with an exogenous port of entry, either through the paranasal sinuses or the ears. Streptococci (usually anaerobe forms such as Peptostreptococcus ) and other anaerobes such as Cutibacterium present as the usual organisms. These organisms usually originate in the sinuses.
IEA may occur as a complication of neurosurgery, with the most likely organism; staphylococci, especially Staphylococcus aureus, and gram-negative bacteria. Infection may also spread inward from osteomyelitis of the skull or fetal monitoring probes applied to the skull during birth. Bacterial SEA forms the major cause of this entity. Most of the time, health care providers cannot find a specific cause of the infection.
What’s the symptoms of an Epidural Abscess?
The symptoms of an epidural abscess depend on the location of the abscess. An epidural abscess may cause the following symptoms:
- Fever
- Pain in the back
- Headache
- Disturbed consciousness
- Unusual sensation throughout the body
- Problems with coordination and movement (Ataxia)
- Trouble walking
- General weakness of muscles in both the arms and legs that worsens over time
- Fatigue and sluggishness
- Nausea and/or vomiting
- Paralysis – inability to move the legs or arms
Diagnosis of Epidural Abscess
Diagnostic tests and exams may include:
- Neurological exam to look for changes in motor and sensory function, vision, coordination and balance, mental status, and in mood or behavior.
- Magnetic resonance imaging (MRI) scan
- Computed tomography (CT) scan
- Tests of a fluid sample from the abscessed area to determine the cause of the infection
- Blood tests to look for germs and other signs of infection
How’s an Epidural Abscess treated?
Typically, a specialist provides antibiotics for the patient to fight the infection that caused the abscess. In surgical cases, a surgeon may need to drain the fluid from the abscess with a needle, to help relieve the pressure. Sometimes, the surgeon may remove it entirely.
References
https://www.hopkinsmedicine.org/health/conditions-and-diseases/epidural-abscess
https://www.ncbi.nlm.nih.gov/books/NBK535450/
