SPINAL ANESTHESIA
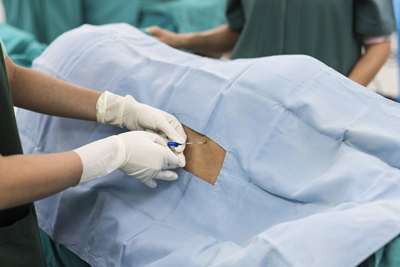
Spinal anesthesia, (also known as intradural block, spinal block, subarachnoid block and intrathecal block) refers to a form of neuraxial anesthesia involving the injection of a local anesthetic or opioid into the space beneath the arachnoid mater containing cerebrospinal fluid (subarachnoid space). The injection requires passing the local anesthetic through a fine needle, usually 9cm in length. Anesthesiologists usually perform this form of anesthesia and it has proven itself as a safe and effective alternative to general anesthesia commonly used in surgeries involving the lower extremities and surgeries below the umbilicus.
The local anesthetic injected into the cerebrospinal fluid provides local anesthesia around a specific region: true analgesia, motor, sensory and autonomic (sympathetic) blockade. If an anesthesiologist administers analgesics (opioid alpha2-adrenoreceptor agonist) without a local anesthetic, it produces localized analgesia (locoregional analgesia): reduced pain sensation (incomplete analgesia), some autonomic blockade (parasympathetic plexi), but absence of sensory or motor block. Due to this absence of sensory or motor block, some patients usually prefer locoregional analgesia to locoregional anesthesia in certain postoperative care settings.
Applications of Spinal Anesthesia
Anesthesiologists commonly use spinal anesthesia either on its own or in addition to sedation or general anesthesia. Surgeries at the lower extremity and below the umbilicus usually require this method, but nowadays, its applications may have extended to surgical procedures above the umbilicus as well as post-op pain blockade. Procedures which apply spinal anesthesia include:
- Caesarean sections
- Urology cases
- Hysterectomy (surgical removal of the uterus)
- Haemorrhoidectomy (surgical removal of haemorrhoids, also referred to as piles)
- Orthopaedic surgery involving the hip, femur, knee joint, ankle and pelvis
- Hernia (inguinal or epigastric)
- Nephrectomy and cystectomy in combination with general anesthesia
- Pain management during vaginal birth and delivery
- Endovascular aortic aneurysm repair
- Vascular surgery on the legs
Pediatricians find spinal anesthesia particularly useful in children with difficult airways and those who do not qualify for endotracheal anesthesia due to the respiratory problems or presence of full stomach.
In Caesarean section, spinal anesthesia provides a better choice as it does not involve a general anesthetic and it reduces the risk of a failed intubation. It also implies the mother remains conscious throughout the delivery.
Spinal anesthesia may also have preference when anesthesiologists cannot intubate patients with severe respiratory diseases such as asthma, pulmonary fibrosis and chronic obstructive pulmonary disease (COPD). It prevents the potential respiratory risks and consequences of intubation and ventilation. It also avoids complications in patients with anatomical/congenital tracheal abnormalities such as tracheo-esophageal fistula.
Risks and Complications
Specialists may encounter certain risks and complications without thorough medical evaluation to ensure zero contraindications and to minimize these risks and complications. These contraindications include:
- Allergic reaction to the anesthetic
- Patient refusal
- Severe aortic stenosis
- Hypovolaemia
- Space occupying lesions of the brain
- Bleeding disorders (such as hemophilia), thrombocytopaenia, or systemic anticoagulation
- Abnormal increase in intracranial pressure
- Local infection or sepsis at the injection site
- Epidural abscess
- Severe hypotension
- Cardiac arrest
- Nerve injuries: cervical radiculopathy, cauda equina syndrome
- Transient neurological symptoms (lower back pain with pain in the legs)
- Infection ( such as meningitis)
- Post-dural puncture headache or post-spinal headache; associated with the needle size and type used.
Serious and permanent complications may not have common occurrence, but usually relate to physiologic effects on the nervous and cardiovascular systems or when the injection has unintentionally entered the wrong site.
Differences Between Epidural and Spinal Anesthesia
Epidural anesthesia refers to a form of anesthesia that involves the injection of a local anesthetic drug into the epidural space through a catheter. This procedure may share certain similarities with spinal anesthesia as they both involve the neuraxial, but one can easily confuse epidural anesthesia for spinal anesthesia. The differences include:
- An anesthesiologist may give an epidural at a cervical, thoracic, or lumbar site, while spinal injection must occur below L2 to avoid injury to the spinal cord.
- Onset of analgesia approximately begins 25-30 minutes in an epidural, while the onset begins approximately 5 minutes in spinal anesthesia.
- Often, an epidural does not require a neuromuscular block, but spinal anesthesia does.
References
Rucklidge M, Hinton C. (2012). “Difficult and failed intubation in obstetrics”. Continuing Education in Anesthesia, Critical Care and Pain.
Serpell, M.G.; Fettes, P.D. W.; Wildsmith, J. AW. (November 1, 2002). “Pencil point spinal needles and neurological damage”.
