SPINAL CORD COMPRESSION
What’s Spinal Cord Compression?
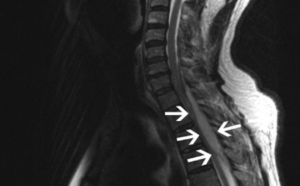
Spinal cord compression, a complex condition that occurs when the spinal cord presents as compressed or squeezed, leading to a wide range of symptoms and potential complications. It can be caused by various factors, including herniated discs, bone spurs, tumors, or spinal stenosis, which narrow the space surrounding the spinal cord and put pressure on the delicate nerves. This compression disrupts the normal flow of nerve signals, resulting in symptoms such as muscle weakness, difficulty walking, loss of sensation, pain, and problems with bladder or bowel control.
In most cases, the source of compression remains located outside the spinal cord (extramedullary), less often within the spinal cord (intramedullary). Compression can overlook as acute (develops in a few hours, occurs during trauma or accompanies a spontaneous epidural hematoma), subacute (develops in days or weeks, caused by a tumor, abscess or hematoma) and chronic (develops over months or years, due to bone or cartilage protrusion into the spinal canal). Symptoms of spinal cord compression may include pain, numbness, weakness, or changes in sensory or motor function in the area affected by the compression. In some cases, spinal cord compression can lead to serious consequences, such as paralysis or organ dysfunction. The diagnosis of spinal cord compression would usually remain based on the patient’s medical history, physical examination, and additional tests such as X-rays, magnetic resonance imaging (MRI), or computed tomography (CT). Treatment would aimed to eliminating compression.
Neurosurgeons play a critical role in the treatment of spinal cord compression, employing their expertise to evaluate each case thoroughly. They assess the underlying cause, the severity of the compression, and the specific symptoms experienced by the patient. Treatment approaches remains tailored to address these factors and provide personalized care. Conservative options may include physical therapy to improve strength and mobility, pain management techniques, and lifestyle modifications to alleviate stress on the spine. In some cases, medications such as anti-inflammatory drugs or corticosteroids might remain prescribed to reduce inflammation and alleviate symptoms.
However, if conservative treatments prove ineffective or if the compression remains severe, surgery might remain necessary to relieve the pressure on the spinal cord. Neurosurgeons perform intricate procedures to decompress the spinal cord by removing the source of compression, such as a herniated disc or tumor. They may also create more space through spinal fusion or laminectomy. Advances in surgical techniques, including minimally invasive procedures, have revolutionized the field, offering benefits such as smaller incisions, reduced tissue damage, and faster recovery times.
Following surgery, rehabilitation and physical therapy remains crucial components of the recovery process. These therapies aim to help patients regain strength, improve mobility, and restore normal function. The spinal cord compression remains a complex condition with diverse causes and symptoms. Neurosurgeons employ their expertise to provide personalized treatment options, ranging from conservative measures to surgical interventions, based on the specific needs of each patient. Timely diagnosis and appropriate treatment remains vital in managing spinal cord compression, as they can alleviate symptoms, restore function, and enhance the overall quality of life.
