PSEUDARTHROSIS
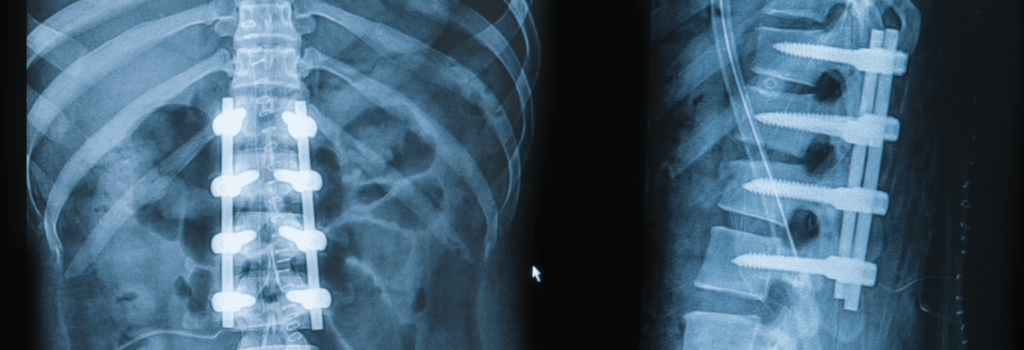
Pseudarthrosis refers to a condition that occurs as a result of an unsuccessful attempted spinal fusion. This condition usually arises with axial or radicular pain, months to years after the operation. Diagnosis of pseudarthrosis occurs based on the clinical presentation and imaging studies, after other causes of persistent pain remain ruled out. The degree of movement noticed on flexion-extension radiographs indicating solid or failed fusion remains a point of controversy. Thin-film CT scans may prove more reliable than radiographs in demonstrating fusion. Metabolic factors, patient factors, use and choice of instrumentation, fusion material, and surgical technique have all influenced the rate of a successful fusion. Treatment of a patient with symptomatic pseudarthrosis involves a second attempt at fusion and may require a different surgical approach from that of the initial surgery as well as the use of additional tools, bone grafts, and osteobiologic agents such as OrthoBlast, mesenchymal stem cells, Norian and proOsteon.
Causes of Pseudarthrosis
Pseudarthrosis may occur in any part of the spine where attempted fusion occurred. The goal with fusion surgery – such as anterior cervical discectomy and fusion (ACDF) and anterior lumbar interbody fusion (ALIF) – involves joining two adjacent vertebrae together as one. However, if the graft material used to allow the fusion to form does not fully create new solid bone tissue, movement will continue in the affected area. Causes of non-unions often involves poor bone healing after performing a procedure, which sometimes happens due to surgical oversights, either with planning before the operation or steps taken during the surgery. However, other cases remain present when a fusion fails to form due to long-term patient habits or conditions. For example, smoking reduces the chances of successful fusion by more than 30 percent. Taking certain steroid medications may also interfere with the body’s natural healing abilities enough to cause an unsuccessful fusion.
Pseudarthrosis remains the leading cause of failed spinal fusions in most cases of spinal surgery. The common causes of this complication include:
- Inadequate surgical technique
- Unrecognized metabolic abnormalities
- Excessive stress across the site of spinal fusion
- Insufficient internal or external stabilization
Risk factors for Pseudarthrosis
If a patient has undergone a spinal fusion surgery and has one or more of the following risk factors, the patient may have increased risk for developing pseudarthrosis:
- If the patient smokes or uses other tobacco products
- Malnourishment/malnutrition
- Obesity
- Hunter syndrome
- Having other metabolic disorders
- Chronic illnesses
- Having uncontrolled diabetes
- Having osteoporosis
- Using steroids for a long period of time
Symptoms of Pseudarthrosis
Depending on where the attempted spinal fusion occurred, pseudarthrosis may cause pain and discomfort in the neck, back, arms or legs. The most common symptom of pseudarthrosis includes continuous pain within the affected area that lingers even after a reasonable period of healing time. Symptoms may also extend to the arms, shoulders, legs or lower extremities if the non-union contributes to nerve irritation. Some patients also experience:
- Numbness and similar sensations such as tingling
- Stiffness in the affected area
- General weakness of the spine, especially in the affected area
In some cases, people with this condition do not experience the symptoms listed above (asymptomatic cases).
Diagnosis of Pseudarthrosis
The specialist will make use of imaging tests – such as an X-ray, computed tomography (CT) scan or magnetic resonance imaging (MRI) scan – to obtain a detailed image of the spine and spinal cord to determine if the patient has pseudarthrosis.
Treatment options
If the patient experiences mild or non-existent symptoms of pseudarthrosis, the surgeon may suggest no further treatment where necessary. Some patients with a non-union respond well to medication, physical therapy, and other non-surgical attempts at pain management. However, the cases may differ sometimes.
In certain cases, the surgeon usually recommends revision surgery as the best treatment option. Before this, the patient may undergo image tests to rule out other potential sources of post-surgery symptoms. In some instances, patients do not notice disruptive symptoms until several months or even years after the initial surgery, which can also make diagnosis difficult. If a second fusion presents as the best option, the surgeon may:
- Use a different type of bone material
- Make corrections to existing errors from the first surgery
- Use a different approach to fusion surgery than initially performed
References
Steinmann JC, Herkowitz HN. Pseudarthrosis of the spine. Clin Orthop Relat Res. 1992 Nov; (284):80-90.
https://www.laspine.com/pseudarthrosis-symptoms-and-causes/
https://www.bonsecours.com/health-care-services/spine-care/conditions/pseudarthrosis
