Stereotactic Brain Tumor Biopsy
What’s Stereotactic Brain Tumor Biopsy?
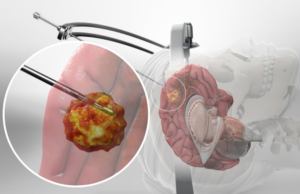
Stereotactic Brain Tumor Biopsy refers to a diagnostic procedure that involves taking a sample of abnormal brain tissue with the use of a biopsy needle to determine the presence of a brain tumor or lesion. This procedure involves the use of a tiny incision that will allow a needle to access the tumor or lesion in the brain and collect a sample for analysis. Stereotactic Brain Tumor Biopsy uses advanced three-dimensional imaging such as MRI and CT scans to make sure that the incision lies precisely in an area where the neurosurgeon can access the tumor without disturbing the surrounding brain tissue. The tissue cells acquired during this minimally invasive procedure can accurately determine the exact kind of brain tumor present. This procedure can also ascertain whether the tumor exists as a cancerous one or not.
A neurosurgeon may prefer stereotactic brain tumor biopsy to the traditional biopsy in cases where the location of the tumor lies in an area difficult to access such as the interior part of the brain. Stereotactic Brain Tumor Biopsy may also prove beneficial for individuals with low anesthesia tolerance.
How do Neurosurgeons carry out Stereotactic Brain Tumor Biopsy?
Stereotactic Brain Tumor Biopsy usually commences with the patient’s head carefully secured in a fixation device. The neurosurgeon will carry out an MRI or CT scan to map out the exact area of the brain tissue where the sampling will occur. The patient may undergo light sedation or application of a topical anesthetic. The neurosurgeon will then shave a section of the patient’s hair and make a very small incision in the skin of the scalp. Drilling of a tiny hole in the skull will occur after which the neurosurgeon, using the imaging scans taken, will guide the biopsy needle into the targeted area of the brain to pull out a tissue sample. After this step, the surgeon will withdraw the needle and close the incision with sutures, glue, or staples.
A Stereotactic Brain Tumor Biopsy procedure typically takes an hour to complete. Examination of the collected brain tissue sample in a pathology laboratory commences immediately after the procedure. The final results from the laboratory usually take three to four days to complete. The neurosurgeon, after consultation with colleagues from radiation and medical oncology, will then discuss the results with the patient and offer the best possible solutions to any abnormality found.
What to expect after Stereotactic Brain Tumor Biopsy?
After a Stereotactic Brain Tumor Biopsy procedure, the incision site may stay protected with the use of a bandage. The patient will stay under observation for a specified time and a nurse will continuously monitor the vital signs of the patient. The neurosurgeon may order an imaging scan after the procedure to ensure that no bleeding or inflammation occurs at the incision site.
The patient may complain of mild nausea or headache after the procedure and the surgeon may administer over-the-counter medication to relieve these symptoms. Patients usually return to their normal activities after a short while.
What’s the Risks and Possible Complications of Stereotactic Brain Tumor Biopsy?
All surgeries come with some sort of possible complications. Complications from a Stereotactic Brain Tumor Biopsy usually do not occur due to their minimally invasive nature. Possible risks of a Stereotactic Brain Tumor Biopsy include infection, intracranial hemorrhage, seizures, stroke, and requiring a second biopsy due to the inability to obtain tissue samples.
References
Bai, Harrison Xiao; Zou, Yingjie; Lee, Ashley M.; Lancaster, Eric; Yang, Li (August 2015). “Diagnostic Value and Safety of Brain Biopsy in Patients With Cryptogenic Neurological Disease”. Neurosurgery. 77 (2): 283–295.
Teixeira MJ, Fonoff ET, Mandel M, Alves HL, Rosemberg S. Stereotactic biopsies of brain lesions. Arq Neuropsiquiatr. (2009) 67:74–7.
Chen CC, Hsu PW, Erich Wu TW, Lee ST, Chang CN, Wei KC, et al. Stereotactic brain biopsy: Single center retrospective analysis of complications. Clin Neurol Neurosurg. (2009) 111:835–9.
Kulkarni AV, Guha A, Lozano A, Bernstein M. Incidence of silent hemorrhage and delayed deterioration after stereotactic brain biopsy. J Neurosurg. (1998) 89:31–5.
Göbel W, Brucker D, Kienast Y, Johansson A, Kniebühler G, Rühm A, et al. Optical needle endoscope for safe and precise stereotactically guided biopsy sampling in neurosurgery. Optics Exp. (2012) 20:26117–26.
